By: @drmelissa.co
Dermatitis is a term that describes general inflammation of the skin. While it is relatively easy to diagnose, discerning the cause can be challenging; typically there are a plethora of factors that come together to cause this condition.
Perioral dermatitis (PD) is general inflammation of the skin around the mouth (“peri” means around and oral refers to the mouth). Symptoms of this condition can include reddened, swollen skin around the mouth and nose, accompanied by itchiness. Sometimes individuals will notice small bumps, hives or breakout-like lesions. Symptoms can come and go, or be persistent. This condition can impact anyone but it is most common in children and females between the ages of 20-45, and is very common in pregnancy or postpartum.
The skin around the mouth and eyes (another common area for dermatitis, called periorbital dermatitis) is more vulnerable because it has fewer oil glands and the skin is thinner. These areas are also more prone to changes in the skin microbiome because they are located close to mucous membranes (the mouth, eyes) which undergo microbial changes as a result of exposures in day-to-day life along with lifestyle factors.
Essentially, the theory is that this skin becomes primed for this condition due to a variety of factors. While healthy skin and a balanced body overall are resilient and can stay healthy despite aggravating factors, internal and external influences come together to weaken the skin, dysregulate the immune system, and ultimately cause this condition.
Internal influences include immune and gut dysfunction, hormonal imbalance, poor diet, high and/or chronic levels of emotional stress, lack of or too much physical activity, poor sleep habits, certain oral medications and organ dysfunction. External factors that can prime the skin for dysfunction include topical products (oral care products, skincare with harsh ingredients like preservatives, retinoids, exfoliants, acids, fragrance, essential oils, stripping cleansers, etc.), certain medications, and environmental factors (dry environment, mould exposure etc.).
Because of the nature of the skin around the mouth and eyes, this area is most vulnerable to shifts in the moisture barrier. A change in moisture balance leads to a change in the pH of the skin, how much oil is produced, and the types of microbes that colonize the area. Eventually these changes may lead to an inflammatory immune system reaction locally in the area. It is this immune system reaction that causes the symptoms listed above.
This condition is multifactorial and treatment is the same; it is rare that only one type of treatment can heal the skin in this area. It also is important to note that recovery takes time and involves consistency with a variety of treatment principles.
In my office, treatment of PD is holistic. We focus on external care of the skin as well as the internal health of the entire system. A good care history is needed; I often spend an hour or more with patients discussing their symptoms, skin history, medical history, lifestyle and diet to paint a picture of why the skin is reacting this way, and what the system needs to heal.
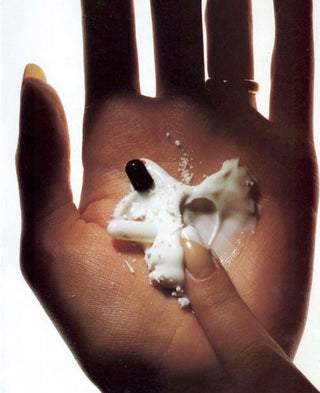
Generally, treatment of this condition takes a minimum of 2-3 months and involves a shift in skincare and oral care first and foremost. Simplification of the skincare routine is required, removing all products with alcohols, exfoliants (scrubs, acids - for a minimum of 2-3 months), scent or essential oils, foaming ingredients, preservatives, and opting for restorative, moisture and pH balancing ingredients. Products with vitamin B3 (niacinamide) introduced very slowly can be helpful, as well as the right type of moisturising lipid blends. A sunscreen with only zinc oxide (avoid titanium dioxide and broad spectrum/chemical sunscreens) can be anti-inflammatory and protective during the day. I also recommend yoghurt masking using full fat, plain organic yogurt over the face for 30 minutes nightly, followed by Manuka honey spot treatment left on overnight. Oral care is also simplified: products with fluoride and sulfates (SLS) are eliminated, and saltwater rinses morning and night are suggested.
When it comes to overall health, treatment becomes more individualised. This can include lab testing in order to uncover potential infections, organ dysfunction, nutritional deficiencies, gut dysbiosis and/or inflammation, and poor immune regulation. A supplement protocol is then created, along with a dietary plan. Typically dietary intervention includes elimination of inflammatory ingredients and promotion of blood sugar balance, nutrient and fibre-dense foods (fruits and vegetables, whole grains), and regular meal timing — particularly a warm, savoury breakfast. Diet also focuses on a reduction or elimination of sugar, dairy, wheat and potentially eggs and soy for at least 30 days. Lifestyle is also a main focus; regular sleep patterns (sleep is when we heal), gentle movement, and stress management are key.
Sometimes, patients opt for a conventional medical approach to PD like steroids or antibiotics. This can be fine, but I always remind them that this is a band aid approach and not curative. While helpful at reducing symptom severity temporarily, it is important not to neglect the whole systems approach while using medications.
In order to heal, consistency is required. Once the skin has healed, we transition into a maintenance approach, where the diet becomes more broad but still nutritious. Skin care is maintained, and lifestyle factors are still front and centre.